- Details
- Last Updated: 09 June 2022 09 June 2022
What is Long COVID?
As of mid-February, 2022, over 78 million cases of COVID-19 have been reported in the U.S., with well over 900,000 deaths(1).
About 10 – 20% of people who have COVID-19, including people who have only mild symptoms, do not fully recover. Many of these people experience a variety of symptoms for many months. This is being called “Long COVID.”
Estimates from January, 2022, are that 20 million or more people in the U.S. have developed Long COVID. In Massachusetts 387,000 people may have Long COVID(2).
Long COVID is a “post-viral” illness.
Where to find more information:
(1) https://www.nytimes.com/interactive/2021/us/covid-cases.html updated Feb. 17, 2022.
Will COVID-19 Lead to ME/CFS?
https://www.frontiersin.org/articles/10.3389/fmed.2020.606824/full
Six-month "long COVID" study reveals 76% suffer lasting symptoms
https://newatlas.com/health-wellbeing/long-covid-study-lancet-lasting-symptoms/
Long-Haul Covid
https://worldneurologyonline.com/article/long-haul-covid/
What is ME/CFS?
Another post-viral or post-infectious illness is ME/CFS. Many people would recognize the name “Chronic Fatigue Syndrome.” The original name is Myalgic Encephalomyelitis, or ME. Today it is known as ME/CFS.
ME/CFS is a serious, debilitating, chronic, multi-system illness that may develop after an infection or other event, such as exposure to toxins, or a physical or stressful trauma. It results in a major impact on the person’s ability to function.
One million to 2.5 million people in the U.S. may have ME/CFS, although many are not officially diagnosed. About 28,000 – 40,000 people in Massachusetts may have ME/CFS.
Where to find more information:
U.S. ME/CFS Clinician Coalition
https://mecfscliniciancoalition.org/about-mecfs/
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
https://www.cdc.gov/me-cfs/index.html
Long COVID and ME/CFS - same or different?
Long COVID and ME/CFS can both result from an infectious viral illness. Long COVID may follow infection with SARS-CoV-2 (a “coronavirus”), while ME/CFS may follow a flu-like illness, infectious mononucleosis (“mono”), or other viral infections.
Both Long COVID and ME/CFS can have many different symptoms and not every person has the same symptoms.
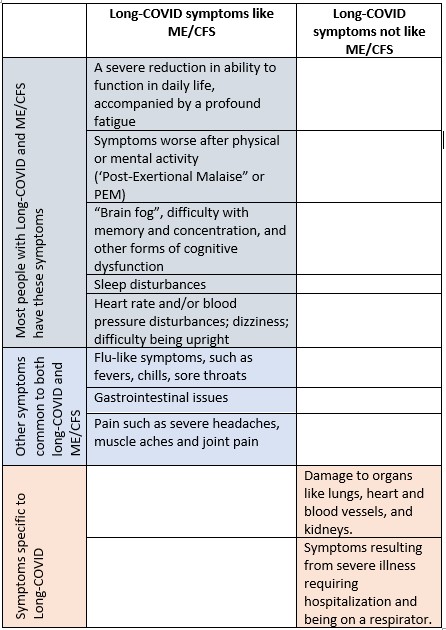
For a diagnosis of ME/CFS, the symptoms must have been present for at least six months at a moderate to severe level. For a diagnosis of Long COVID, symptoms will still be present after 28 days to 3 months. If symptoms are still present after six months, a diagnosis of ME/CFS should be considered in the differential diagnosis of long COVID patients.
Where to find more information:
Characterizing Long COVID…
https://www.medrxiv.org/content/10.1101/2020.12.24.20248802v2.full.pdf
Will COVID-19 Lead to ME/CFS?
https://www.frontiersin.org/articles/10.3389/fmed.2020.606824/full
Opportunities for joint research (ME/CFS and Long COVID)
Some research is now being done on long COVID and ME/CFS.
One such study that is accepting patients is https://youandmeregistry.com/.
Many researchers are now studying the effects of Long COVID. Here is one example:
Six-month "long COVID" study reveals 76% suffer lasting symptoms
https://newatlas.com/health-wellbeing/long-covid-study-lancet-lasting-symptoms/
Lessons learned from ME/CFS
Many ME/CFS patients have been chronically sick with a post viral-like illness. They have learned some lessons that may be helpful to patients who are just developing similar symptoms.
Treatment/management – treat symptoms, learn pacing
Doctors are just starting to learn more about Long COVID. Even if your doctor doesn’t have all the answers, s/he should listen to you and take your concerns seriously.
Your doctor should be a partner with you to help you feel and function better. The most bothersome symptoms can often be treated first. Learning about and practicing pacing will often be very helpful and should be started as early as possible.
Pacing - Do your best to avoid “pushing through” fatigue
Pacing your activity, to the extent possible, is important to allow your body to recover and heal. Try not to do too much to the extent that it will cause you to get worse. Listen to what your body is telling you and take rest periods if you can, preferably lying down, after periods of activity. Make a choice about what is essential and what is not, and, if possible, ask for help from those willing to take some of the burden off your shoulders. Be sure that a program of “graded exercise” to “recondition” will not be beyond your energy tolerance and make you worse. It is challenging to avoid going beyond one’s individual energy limit because it can vary from day to day.
“The key to successful adjustment in ME/CFS and fibromyalgia is pacing, which provides an alternative to the cycle overdoing followed by forced rest (‘push and crash’.) By first understanding the limits imposed by illness and then adjusting to live within them, people can reduce symptoms, decrease the frequency and severity of relapses, and experience greater stability. Pacing also provides the foundation for gradual expansion of limits.” Source: Bruce Campbell, The ME/CFS & Fibromyalgia Self-Help Program, cfsselfhelp.org.
Take one day at a time
It is frightening to not be getting better, and not know how and when you will recover.
You will have some bad days and some better days. Although the outcome of long COVID is not yet known, with time, the majority of people with ME/CFS gradually improve, although usually not to their pre-illness level.
Family members, friends, and even health care providers may question or not understand your illness, especially if your symptoms vary over time. They need to learn you are really sick and can’t do everything you used to do. You should not be blamed, nor should you blame yourself – no one wishes to get sick. Instead, seek treatment and support from those who care for you, tell them how you are feeling and how they can help. Seek any potential outside support. You may need to educate others as well as yourself, as you learn more.
How to work with your doctor
Try to organize your thoughts before your visit. Write them down if you need to. If you are having “brain fog” tell the doctor that and ask for understanding. Take someone you trust to go with you to help you remember what your doctor has said.
Explain your illness and symptoms to your doctor. You may not have time to tell your whole story or list all your symptoms during your appointment, so start with the most important things. Be sure your doctor takes time to hear you.
Listen to what the doctor has to say about his or her plan to treat you, and don’t hesitate to ask questions. When the appointment is over, you should leave knowing how the doctor is planning to help you.
If you find the doctor is not helping you or is not explaining things, and you don’t have a feeling of confidence, you may need to find another doctor.
Where to find more information:
Tips on how to get the most out of a doctor's visit https://www.massmecfs.org/working-with-your-me-cfs-doctor?start=2
If your doctor does not believe you, find another doctor
All patients deserve to be believed, and treated respectfully. Your doctor can likely help you deal with specific symptoms, at least, and should be looking to see if you have other conditions which might be treatable. If you are not comfortable with how you are being treated, you may need to look for another provider.
Where to find more information:
About ME/CFS
https://www.massmecfs.org/cfids-me-cfs
Find support
If your family, friends, and health care providers are not supportive, you may need to look elsewhere for support. Many long COVID patients have joined local or national groups where they find they are not alone.
Where to join a group or find more information (this is just a sample):
In Massachusetts:
https://www.c19recoveryawareness.com/
National groups:
https://www.facebook.com/groups/205703087068863
https://www.facebook.com/groups/longcovid/
https://www.wearebodypolitic.com/covid19
If you feel despondent…
Getting sick with ME/CFS and Long Covid can be extraordinarily difficult, physically, and can result in loss of the ability to work and socialize and care for oneself. This can be emotionally devastating. Some people lose hope and feel like their lives are lost, even if they are still alive.
If you or someone you know is in immediate danger please call 911 in the USA or your local emergency services in your country. If you or someone you know is at risk for suicide in the U.S., call the U.S. National Suicide Prevention Lifeline at 800-273-8255, or text HOME to 741741.
Additional resources:
In the United States, please go to https://SpeakingOfSuicide.com/resources for additional resources.
Here is a link to international suicide prevention resources:
https://www.iasp.info/resources/Crisis_Centres/
What if you can’t work?
If you can’t continue your regular work, you may first ask for job accommodations from your employer. If you cannot get accommodations that allow you to work, or you become too sick to work and trying to continue makes you worse, you should apply for disability assistance, either through your employer or Social Security.
You should not feel ashamed if you can’t work – anyone can get sick through no fault of their own. You need income and medical insurance so that you can get better.
Applying for disability can be a long and frustrating process. You may need someone to help you prepare your application. You must show through records from your doctor that you have a serious and chronic medical illness, and that you cannot carry out work and everyday tasks. Write down examples of what you can and cannot do on a good day and on a bad day. Ask your doctor to put these into your medical record.
People with post-viral illness are likely to be rejected for disability at first, but you may succeed if you keep trying.
Where to find more information:
MassMECFS Disability Home Page
https://www.massmecfs.org/disability
More about ME/CFS
Diagnosing ME/CFS
These symptoms are required for a clinical diagnosis of ME/CFS:
- a substantial reduction in daily functioning including profound fatigue,
- post-exertional malaise,
- unrefreshing and disordered sleep,
- and either cognitive impairment or orthostatic intolerance.
Additional symptoms which often occur are: flu-like symptoms, sensory sensitivity, pain, recurrent headaches, and gastrointestinal disturbances.
The description below from the Institute of Medicine (IOM) report is more complete and informative for people who are not familiar with medical terms:
Three symptoms and at least one of two additional symptoms are required for diagnosis. The three required symptoms are:
1. A substantial reduction or impairment in the ability to engage in pre-illness levels of activity (occupational, educational, social or personal life) that
- lasts for more than 6 months
- is accompanied by fatigue that is:
- often profound
- of new onset (not life-long)
- not the result of ongoing or unusual excessive exertion
- not substantially alleviated by rest
2. Post-exertional malaise (PEM)* – worsening of symptoms after physical, mental or emotional exertion that would not have caused a problem before the illness. PEM often puts the patient in relapse that may last days, weeks, or even longer. For some patients, sensory overload (light and sound) can induce PEM. The symptoms typically get worse 12 to 48 hours after the activity or exposure and can last for days or even weeks.
3. Unrefreshing sleep* – patients with ME/CFS may not feel better or less tired even after a full night of sleep despite the absence of specific objective sleep alterations.
And at least one of the following two must also be present:
1. Cognitive impairment* – patients have problems with thinking, memory, executive function, and information processing, as well as attention deficit and impaired psychomotor functions. All can be exacerbated by exertion, effort, prolonged upright posture, stress, or time pressure, and may have serious consequences on a patient’s ability to maintain a job or attend school full time.
2. Orthostatic intolerance – patients develop a worsening of symptoms upon assuming and maintaining upright posture as measured by objective heart rate and blood pressure abnormalities during standing, bedside orthostatic vital signs, or head-up tilt testing. Orthostatic symptoms including lightheadedness, fainting, increased fatigue, cognitive worsening, headaches, or nausea are worsened with quiet upright posture (either standing or sitting) during day-to-day life, and are improved (though not necessarily fully resolved) with lying down. Orthostatic intolerance is often the most bothersome manifestation of ME/CFS among adolescents.
*The frequency and severity of these symptoms need to be evaluated. The IOM committee specified that “The diagnosis of ME/CFS should be questioned if patients do not have these symptoms at least half of the time with moderate, substantial, or severe intensity.”
Other causes for these symptoms should be ruled out.
Diagnosis should also include a workup to see if there are other causes for symptoms which might be treatable.
Where to find more information:
U.S. ME/CFS Clinician Coalition
https://mecfscliniciancoalition.org/about-mecfs/
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
https://www.cdc.gov/me-cfs/index.html
Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Redefining an Illness (2015)
https://www.nap.edu/catalog/19012/beyond-myalgic-encephalomyelitischronic-fatigue-syndrome-redefining-an-illness
Treating and Managing ME/CFS (The Basics)
Here are the main points about treating and managing ME/CFS from a group of expert ME/CFS clinicians. If you have lingering symptoms after COVID-19 infection, and some of your symptoms seem similar to ME/CFS, this information might be useful to you and your doctor.
This is an important point these expert clinicians want all doctors to understand:
“In the past, ME/CFS has been characterized as a syndrome of medically unexplained fatigue responsive to talk therapy and graded exercise. But scientific advances are revealing a complex, multisystem disease involving neurological, immunological, autonomic, and energy metabolism impairments. There is a critical need for a different approach to management of the disease and accompanying comorbidities.”
Here is how these expert ME/CFS clinicians suggest doctors should treat ME/CFS:
1. Validate the patient experience and educate about the disease.
The most important thing that a medical provider can do is to validate the illness for the patient and the patient’s family. Explain that ME/CFS is a serious medical illness and is not laziness, depression, or a psychosomatic disorder.
2. Address impaired function and provide support as needed.
By definition, patients with ME/CFS have significant disability. Patients may need help in obtaining accommodations for school and work or when applying for disability. They may also need parking permits, assistive devices, and/or home health aides.
3. Educate patients about pacing to prevent or minimize PEM.
Pacing is an individualized approach to managing physical, cognitive, and emotional energy within a patient’s specific limits by carefully planning where and how to spend their available energy. It is a critical tool to prevent and/or reduce PEM. Activity logs and heart rate and activity monitors can be used to help patients understand when they are overdoing their specific energy limits.
4. Treat/manage symptoms.
While there are no treatments approved specifically for ME/CFS, a number of different pharmacological and non-pharmacological treatments can help reduce the severity of symptoms.
Drugs should be started at low doses and increased slowly to avoid triggering drug sensitivities common in ME/CFS.
5. Treat Comorbid Conditions.
As listed earlier, a number of conditions may be comorbid (exist at the same time) with ME/CFS. Treating these comorbid conditions using the appropriate standard of care will not cure ME/CFS but it may improve the patient’s quality of life.
Where to learn more:
Here is a short handout written by expert ME/CFS clinicians that you can print and take to your doctor:
DIAGNOSING AND TREATING MYALGIC ENCEPHALOMYELITIS/CHRONIC FATIGUE SYNDROME (ME/CFS)
– U.S. ME/CFS CLINICIAN COALITION –
Version 2, July 2020
https://drive.google.com/file/d/1SG7hlJTCSDrDHqvioPMq-cX-rgRKXjfk/view